Most people only think about gums disease when something feels wrong. A little bleeding after brushing, some tenderness along the gumline, or breath that just won’t quit—these things are easy to brush off as minor inconveniences. But your gums are often the first place your body signals that something more serious is developing.
Understanding Gum Disease
Gum disease, also called periodontal disease, is a bacterial infection of the tissues that support your teeth. It develops in stages, starting with gingivitis and potentially progressing to periodontitis.
Gingivitis
Gingivitis is the earliest and mildest form. At this stage, bacteria in plaque—the sticky film that builds up on your teeth—irritate the gum tissue, causing inflammation. The damage is limited to the gums themselves, which means it’s still fully reversible with proper care.
Many people have gingivitis without knowing it. There’s usually no pain, and the signs can be subtle. That’s what makes it so easy to overlook.
Periodontitis
Left untreated, gingivitis can advance to periodontitis. At this stage, the infection spreads below the gumline, damaging the bone and connective tissue that hold your teeth in place. Pockets form between the gums and teeth, creating an environment where bacteria thrive and the damage compounds over time.
Periodontitis cannot be reversed—only managed. That distinction is exactly why early detection matters so much.
Common Warning Signs of Gum Disease
The earlier you spot these signs, the more treatment options you have. Here’s what to watch for:
Bleeding Gums
Healthy gums don’t bleed. If you notice blood when brushing or flossing, even occasionally, that’s your body flagging inflammation. Some people assume it means they’re brushing too hard, but in most cases, it points to gingivitis. Don’t ignore it—address it.
Persistent Bad Breath
Everyone has bad breath now and then. Persistent bad breath, or a bad taste in your mouth that won’t go away, is a different story. It often signals a buildup of bacteria in areas that regular brushing can’t reach, particularly beneath the gumline or in deepening gum pockets.
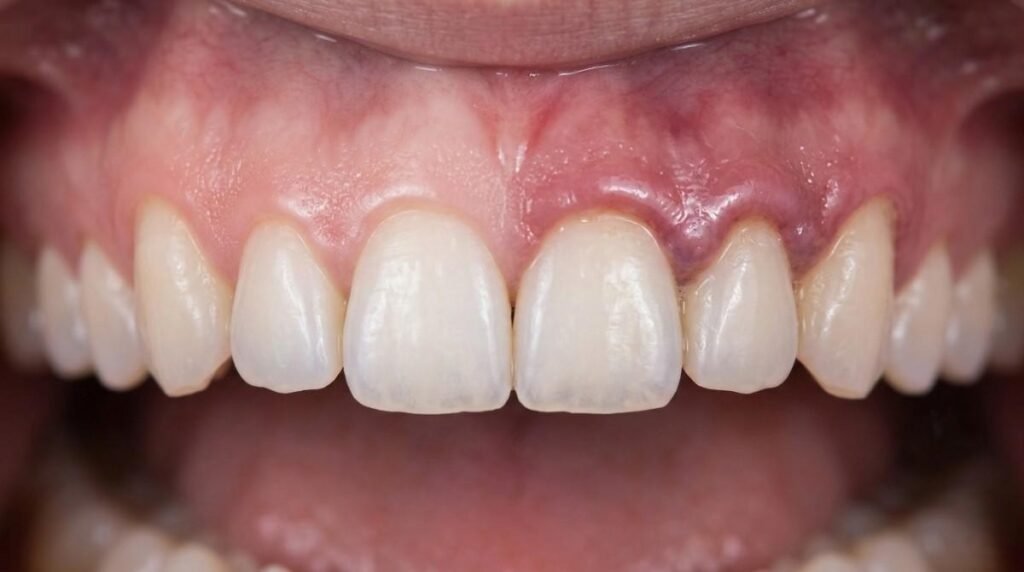
Red, Swollen, or Tender Gums
Healthy gum tissue is firm and pale pink. Gums that look red or puffy, or feel sore when touched, are showing classic signs of inflammation. This is one of the earliest visual indicators of gingivitis and shouldn’t be dismissed as normal.
Receding Gum Line
If your teeth appear longer than they used to, your gums may be pulling away from the tooth surface. Gum recession exposes the roots of your teeth, increasing sensitivity to hot and cold temperatures. It also creates pockets where plaque and bacteria accumulate—accelerating the progression of disease.
Loose or Shifting Teeth
As periodontitis advances, the bone supporting your teeth begins to deteriorate. This can cause teeth to become loose, shift position, or change the way your bite feels. By the time this symptom appears, the disease has usually progressed significantly.
Increased Tooth Sensitivity
Sensitivity isn’t always about enamel erosion. When gum recession exposes root surfaces, those areas have far less protection against temperature changes and pressure. Sudden or worsening sensitivity can be a sign that your gums are receding—even if it’s not yet visible.
Why Early Detection Matters
Oral health doesn’t exist in isolation from the rest of your body. Research has established links between gum disease and several systemic conditions, including heart disease, type 2 diabetes, and respiratory illness. The bacteria involved in periodontal infections can enter the bloodstream, triggering inflammatory responses elsewhere in the body.
For people already managing diabetes, the relationship runs in both directions—gum disease can make blood sugar harder to control, and elevated blood sugar accelerates gum disease. Similarly, studies have found associations between periodontitis and increased cardiovascular risk, though the mechanisms are still being studied.
Beyond systemic health, the practical costs of late-stage treatment are significant. Treating gingivitis typically involves a professional cleaning and improved home care. Treating advanced periodontitis involves scaling and root planing, antibiotic therapy, and in some cases, oral surgery to repair or regenerate damaged tissue. Early intervention is not only more effective—it’s far less invasive and expensive.
At-Home Prevention Tips
You have more control over your gum health than you might think. Consistent daily habits go a long way in preventing disease from developing in the first place.
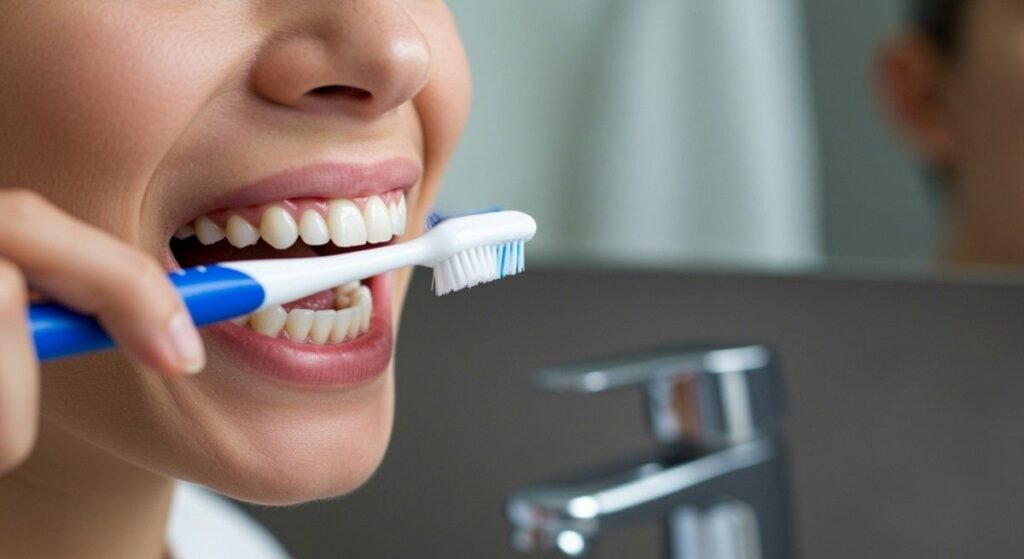
Brush Effectively—Not Just Frequently
Brushing twice a day is the baseline, but technique matters. Use a soft-bristled toothbrush and hold it at a 45-degree angle to your gumline. Gentle circular motions clean more effectively than aggressive scrubbing, which can actually damage gum tissue over time. Electric toothbrushes have been shown to remove more plaque than manual ones, making them a worthwhile upgrade.
Floss Every Day
Flossing isn’t optional if you’re serious about gum health. It removes plaque and food debris from between teeth and just below the gumline—areas a toothbrush simply can’t reach. If traditional floss is difficult to manage, interdental brushes or water flossers work just as well.
Watch Your Diet
Sugar feeds the bacteria that produce acid and plaque. Diets high in refined carbohydrates and sugar accelerate plaque buildup and gum inflammation. On the flip side, a diet rich in vitamins C and D supports gum tissue repair and immune response. Staying hydrated also helps, since dry mouth reduces saliva—your mouth’s natural defense against bacteria.
Quit Smoking
Smoking is one of the strongest risk factors for gum disease. It impairs blood flow to the gums, masks early symptoms like bleeding, and significantly slows healing. Smokers are much more likely to develop periodontitis and respond poorly to treatment. Quitting at any stage reduces that risk.
Use an Antibacterial Mouthwash
A fluoride or antibacterial mouthwash used after brushing and flossing helps reduce bacterial load in areas that are still difficult to reach. It’s not a substitute for mechanical cleaning, but it adds a meaningful extra layer of protection.
When to See a Dentist
Home care is essential, but it’s not the whole picture. Modern dentistry can save your teeth. Professional dental visits allow your dentist to assess gum pocket depth, check for bone loss, and remove hardened tartar (calculus) that can’t be removed by brushing alone.
What to Expect at a Checkup
During a routine visit, your dentist or hygienist will probe around each tooth to measure gum pocket depth. Healthy pockets measure 1–3mm. Anything deeper may indicate disease activity. X-rays help detect bone loss that isn’t visible during a clinical exam.
Professional Treatment Options
For early-stage gum disease, a professional cleaning—or scaling and root planing for more advanced cases—is typically the first line of treatment. This deep-cleaning procedure removes plaque and tartar from below the gumline and smooths root surfaces to discourage bacterial reattachment.
In more advanced cases, antibiotic therapy may be prescribed alongside cleaning. For patients with significant bone or tissue loss, oral surgery in Salt Lake City may be necessary—procedures such as flap surgery, bone grafting, or soft tissue grafts can help restore the structures that support your teeth. These interventions are highly effective, but they’re most successful when the disease is caught before too much damage has occurred.
How Often Should You Go?
Twice a year is the standard recommendation, but people with a history of gum disease may benefit from more frequent visits—typically every three to four months. Your dentist will recommend a maintenance schedule based on your individual risk factors.
Conclusion
Gum disease is common, but it’s not inevitable. Catching it at the gingivitis stage means you can reverse it entirely. Catching it at the periodontitis stage means you can stop it from progressing. Ignoring it means facing more complex, costly, and invasive treatment down the road.